Lensometer

This product has not been manufactured in many years and is now obsolete. Parts and service are no longer available. The User Guide is available for download in the "Instructions" tab below.
-
Details
-
Instructions
-
Related Items
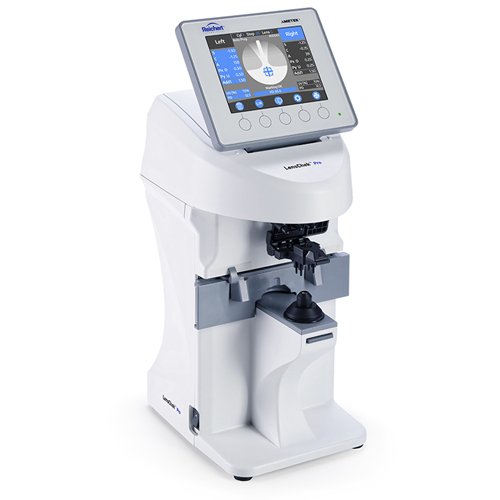
LensChek® Pro
Digital Lensometer® with PD + UV
The all-new LensChek Pro Digital Lensometer with PD + UV, part of the VisionChek Digital Exam Suite, combines technology and simplicity of lens measurement, at the core of your exam.
LensChek® Plus
Digital Lensometer®
The LensChek® Plus - Digital Lensometer®, part of the VisionChek™ Digital Exam Suite, combines technology and simplicity of lens measurement, at the core of your exam.
